University scientists found that a test used to monitor blood sugar can be ineffective for those with the sickle cell trait. The study, published in the Journal of the American Medical Association February, tested African American sickle cell trait carriers to see how carrying the trait affects results of the Hemoglobin A1C test, a common blood glucose test. Researchers found the sickle cell trait has a significant effect on the test’s results, which implies that sickle cell trait carriers are more likely to be misdiagnosed and standard medical tests may produce different results for different races.
The test dates back to the 1980s. During the 1990s, different institutes realized they were receiving different results on the test, said Joseph Aloi, professor of endocrinology and metabolism at the Wake Forest School of Medicine, who co-authored a response to the study.
Because of the differing results, the institutes formed a group to develop a national standard for the test measurements.
A1C tests have since become the standard for measuring blood glucose, Aloi said. Mary Lacy GS, doctoral candidate in epidemiology and the study’s lead author, said that the A1C test has been used to diagnose diabetes since 2010. Before then, it was used to monitor glucose control in people who had already been diagnosed with diabetes. “(The A1C) has turned out to be an incredibly powerful test, both for the diagnosis and treatment of diabetes,” said Anthony Bleyer, professor of nephrology at the Wake Forest School of Medicine, in an interview with National Public Radio.
The study used the largest sample size yet to analyze the effect that the sickle cell trait has on blood glucose levels in African Americans. The researchers analyzed the A1C results of 4,620 individuals in two studies. They found that, despite other medical tests showing similar blood sugar results, individuals carrying the sickle cell trait had a lower A1C reading than those without. This implies that the trait leads to a lower measure of blood sugar for these patients.
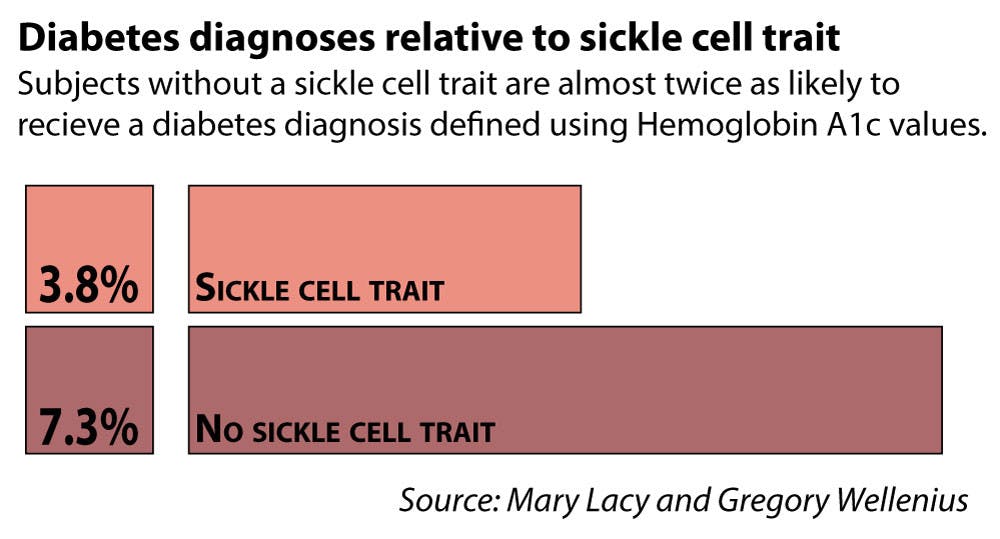
“We also found that, when using standard A1C cutoffs to screen for disease prevalence, we identified 40 percent fewer cases of prediabetes and 48 percent fewer cases of diabetes in individuals with sickle cell trait than in those without sickle cell trait,” Lacy said.
The implications for these findings are numerous as they suggest the A1C test may underestimate the risk for diabetes in those who carry the sickle cell trait, Lacy said. This could subsequently lead to inaccurate patient information and even misdiagnoses for carriers. Sickle cell trait carriers are at a higher risk for these discrepancies than others, especially African Americans — 8 to 10 percent of whom carry the trait, according to the study. Scientists were aware from numerous studies that the A1C did not measure blood sugar in African Americans as accurately as it did in those of European descent, but researchers have only now put the findings into context, Aloi said.
Scientists involved with the study believe that this test will open new doors for more accurate diagnoses for sickle cell trait carriers. Though one in 12 African Americans carry the sickle cell trait, most are not aware they have it, Lacy said. She also urges people to talk with their doctors about their results.
“We need to be able to have a measurement that brings in all of these different factors,” Aloi said. Other factors, such as iron deficiency, anemia and liver disease, will also subtly change the results of the A1C test. The main message for health care providers is that they need to realize there are pitfalls in the information they are given, Aloi said. If a patient, namely one who carries the sickle cell trait, says their blood sugar is different than what the A1C indicated, the difference may be attributed to race, he added.